In today's healthcare environment, minimizing contamination risks is a critical priority. Understanding how hospitals reduce contamination risks is essential for patient safety. Contaminants can lead to infections, which may complicate recovery and extend hospital stays.
Hospitals implement best practices to create a cleaner environment. These practices include thorough cleaning procedures, regular training for healthcare staff, and the use of advanced sterilization techniques. The role of leadership is crucial in enforcing these standards. However, not all hospitals consistently apply these methods.
Challenges still exist in maintaining cleanliness. Staff shortages and budget constraints can hinder effective implementation. Continuous evaluation and adaptation of strategies are necessary to address these issues. This guide explores effective practices that hospitals can adopt to enhance safety and reduce risks.
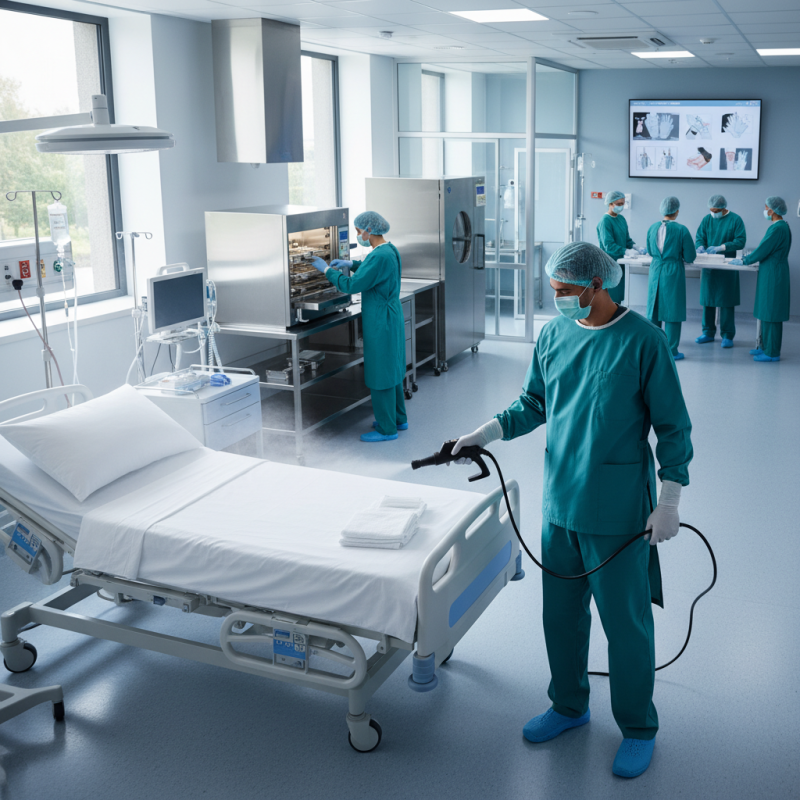
Infection control in hospitals is crucial to patient safety. Effective practices minimize contamination risks significantly. Hospitals must prioritize hand hygiene. Staff should wash hands frequently and correctly. This simple act can prevent the spread of many infections. Regular training on proper handwashing technique is essential.
Environmental cleanliness plays a vital role. Disinfecting surfaces daily helps reduce pathogens. However, challenges arise. Some areas are harder to clean. Equipment can harbor bacteria. Regular audits can identify these problem spots. Contingency plans should be in place for persistent issues.
Isolation protocols must be adhered to strictly. Patients with known infections need designated areas. Yet, balancing space and isolation can be difficult. Staff education on the importance of isolation is vital. They must understand that every practice matters in infection prevention.
Effective hand hygiene protocols are essential in reducing contamination risks in hospitals. Hospitals must prioritize the cleanliness of hands among healthcare professionals. Regular handwashing with soap and water or the use of alcohol-based hand sanitizers can significantly decrease the spread of infections. Staff should wash hands before and after patient contact. This simple act can make a huge difference.
Training programs play a crucial role in promoting proper hand hygiene. Staff should receive periodic training on techniques and importance. Visual reminders can serve as effective prompts in restrooms and patient areas. However, compliance can falter. Some healthcare workers may overlook hand hygiene due to time pressures or forgetfulness. Regular audits and feedback can help address these challenges, ensuring that hand hygiene becomes a habitual practice.
Creating a culture of accountability is vital. Engaging all levels of staff fosters a shared responsibility for infection control. Events like hand hygiene awareness days can promote discussion. Nonetheless, hospitals must reflect on their strategies. Are they recognizing successes? Are they addressing failures effectively? Continuous improvement is necessary for maintaining high standards of hygiene and patient safety.
This bar chart displays the compliance rates for hand hygiene protocols in different hospital departments, reflecting best practices in reducing contamination risks.
Advanced sterilization techniques are crucial in hospitals to minimize contamination risks. Effective methods include steam sterilization, which employs high temperatures and pressure to eliminate pathogens. This process is reliable, yet it requires strict monitoring to ensure proper function and avoid any lapses in sterilization. Regular training for staff is necessary but often overlooked. It is essential to maintain competency in these practices.
Another effective technique is the use of ethylene oxide gas. This method targets sensitive medical equipment that cannot withstand high heat. However, the process demands careful handling due to its toxic properties. Facilities must ensure that staff is fully educated on safety protocols. Even with advanced methods, there can still be gaps that lead to oversight, thus raising questions about accountability.
Innovative technology, like ultraviolet (UV) light systems, is revolutionizing sterilization. UV light effectively disinfects surfaces in rooms and operating theaters. Yet, implementation requires proper evaluations to confirm its efficacy for specific pathogens. Regular audits and checks are vital to assess the effectiveness of all sterilization methods. A proactive approach ensures that hospitals continually adapt and improve practices, responding to emerging threats in healthcare environments.
| Practice | Description | Frequency | Effectiveness (%) |
|---|---|---|---|
| Use of Autoclaves | High-pressure steam sterilization of instruments. | Daily | 98% |
| Surface Disinfection | Frequent cleaning of high-touch surfaces. | Every 2 hours | 95% |
| Hand Hygiene | Usage of hand sanitizers and gloves. | Before/after each patient | 90% |
| Advanced Cleaning Protocols | Using specialized agents for deep cleaning. | Weekly | 97% |
| Air Filtration Systems | Regular filtration and sterilization of air in patient areas. | Monthly | 99% |
Infection control in hospitals is critical. Educating both patients and staff is essential for reducing contamination risks. Comprehensive training can help everyone understand their roles in maintaining a clean environment.
Tips: Regular workshops can keep staff informed. They should explore protocols and share experiences. Encourage questions to foster a collaborative culture. When staff feel supported, they are more likely to adhere to best practices.
Patient education is equally important. Simple, clear information about hand hygiene and infection prevention can make a difference. Visual aids, like posters, can enhance understanding. Engaging patients in their care empowers them to participate actively, reducing the risk of infections.
Tips: Use multimedia tools for patient education. Short videos or interactive sessions can improve retention. Encouraging patients to voice concerns can also help identify gaps in awareness. It creates an environment where vigilance is shared.
Monitoring and evaluating contamination risks is crucial in today’s hospitals. Regular assessments help identify vulnerabilities in protocols. In a 2021 study, hospitals that conducted bi-monthly audits reported a 30% decrease in infection rates. This shows that proactive measures pay off.
Routine monitoring includes swabbing surfaces and air quality checks. A recent report indicated that 10% of clinical surfaces tested positive for pathogens. This highlights areas needing immediate attention. Staff education also plays a role. Continuous training ensures that team members are aware of evolving practices and risks.
Yet, challenges persist. Many facilities lack adequate resources for consistent monitoring. A survey found that 40% of hospitals perform evaluations less frequently than recommended. This gap may lead to unnoticed risks. Regular feedback loops could enhance transparency. A culture of accountability must be fostered to address these issues effectively.
: Advanced sterilization techniques minimize contamination risks in hospitals. They are crucial for ensuring patient safety.
Steam sterilization uses high temperatures and pressure to kill pathogens. It is reliable but needs strict monitoring.
Ethylene oxide gas targets sensitive equipment but is toxic. Staff must be trained on safety protocols to handle it properly.
Regular staff training ensures competency in sterilization practices. It’s often overlooked but essential for effective infection control.
UV light disinfects surfaces in rooms and operating theaters. Proper evaluations are required to confirm its efficacy against pathogens.
Educating patients about hygiene and infection prevention is vital. It empowers them to actively participate in their care.
Regular workshops encourage staff collaboration and discussion. This creates an environment where everyone feels supported in best practices.
Short videos and interactive sessions can improve patient understanding. Visual aids like posters also enhance awareness.
Even advanced methods can have gaps leading to oversight. Accountability is a concern that requires ongoing reflection.
Regular audits assess the effectiveness of sterilization methods. They ensure hospitals can adapt and improve in response to emerging threats.
In the pursuit of how hospitals reduce contamination risks, effective infection control remains paramount. Best practices involve implementing rigorous hand hygiene protocols, which require both staff and patients to adhere to comprehensive handwashing guidelines. Additionally, the utilization of advanced sterilization techniques, including innovative disinfection methods, plays a crucial role in minimizing the spread of pathogens.
To further support these efforts, integrating patient and staff education programs helps to foster a culture of safety and awareness regarding infection prevention. Regular monitoring and evaluating of contamination risks are essential to ensure that these practices remain effective and adaptive to emerging challenges. By focusing on these strategies, hospitals can significantly enhance their infection control protocols, thereby safeguarding the health of patients and staff alike.

 RosMed Medical
RosMed Medical